Keywords
Ageing, implementation, evaluation, ICOPE, intrinsic capacity
Whilst life spans are increasing globally, health spans are not. There is a critical need for “Healthy Ageing”, particularly in low- and middle-income countries (LMICs). This study aims to adapt the WHO Integrated Care of Older People (ICOPE) framework and implement and evaluate a contextually-appropriate, “health check-up” for older people, incorporating community interventions to promote healthy ageing within the existing public healthcare system in Zimbabwe.
Keeping Older people healthy, deSigning and evaluating effective HEalth Services to maintain functional AbIlity (KOSHESAI) is a prospective hybrid type 2 implementation-effectiveness study. Its objective is to create and implement a community-based, non-specialist assessment and management of age-related impairments in intrinsic capacity and functional ability in older Zimbabweans. The intervention will be delivered in local primary healthcare clinics in urban Harare and rural Murehwa district, targeting 732 adults age ≥65 years in each setting. Participants will be screened and assessed for impairments across seven intrinsic capacity domains. Interventions include immediate on-the-spot care, personalized health advice, patient-facing written guidance, specialist referrals, and home visits if individuals are home-bound. Two types of Community-based Healthy Ageing Peer-to-peer Support (CHAPS) groups will be developed for those with identified deficits, focusing on ‘healthy ageing’ and ‘healthy minds’ (if cognitively impaired). Baseline and 4-month follow-up data, will assess the proportion who access appropriate care. Secondary outcomes include diagnostic accuracy, impairment prevalence, clinical improvements, process evaluation (coverage, fidelity, acceptability), and cost metrics. Quantitative data will use descriptive statistics and before-after comparisons; qualitative data will use thematic analysis and elements of the Framework Method, integrating identified theoretical frameworks. A convergent parallel design will triangulate findings.
The adaptation, implementation and evaluation of the WHO ICOPE framework will inform the development of a ‘Healthy Ageing Intervention Toolkit’, providing a structured, comprehensive, person-centred assessment and management approach, ready for scale-up across sub-Saharan Africa.
Thanks to medical advances, people are living longer. In these added years of life, older people want to stay healthy, independent and active - this is called ‘healthy ageing’. However, healthcare services are not currently designed to meet the needs of a rapidly ageing population. The World Health Organization (WHO) describes healthy ageing as an older person’s ability to walk, see, hear, and function mentally within the place they live. To proactively plan ways of providing healthcare, we aimed to develop and test a ‘Healthy Ageing Check-up’, run by local non-specialists, where older people can be assessed and managed to maintain their health and function.
We have worked closely with a range of stakeholders, including older people themselves, to develop and test a health check-up for people aged 65 years and older, in Zimbabwe. The check-up we have designed will assess, for walking, balance, nutrition, memory, mood, eyesight, hearing and bladder function. We will offer personalised advice, practical solutions, facilitate specialist referral for identified problems, and invite older people to take part in the community peer-to-peer support groups (CHAPS). We will test how well the roll-out of this system of health checks works, for example how often we identify a health problem, how often we can offer a solution and, after 4 months, how frequently the older person has taken up recommended referrals. We will calculate how much it costs to provide and receive the health check-ups and care. Throughout, we will gather feedback about the health check-up programme, so that we can refine and improve the process.
We have worked with local communities to develop the peer-support groups, each led by a community champion who we have trained. Peer-support groups will bring together older people with similar conditions to enable group-based self-management and peer support.
The findings from this study will show us what works best for older adults in Zimbabwe. This information will be used to develop a ‘Healthy Ageing Intervention Toolkit’ to guide person-centred assessment and management of older people, ready for scale-up. We will share our results, and resources with the Zimbabwe Ministry of Health, local partner organizations that work with older adults, both WHO Zimbabwe and WHO global, as well as with other international health organizations. Our hope is that this research will lead to reduced ageism, and improved and more respectful healthcare for older people, promoting healthy ageing practices not only in Zimbabwe but across Africa.
Ageing, implementation, evaluation, ICOPE, intrinsic capacity
The study builds on the WHO ICOPE approach to offer a pragmatic community-based intervention delivered by non-specialists to promote healthy ageing in both urban and rural settings.
A prospective hybrid type 2 implementation-effectiveness study design will be complemented by a detailed process and cost evaluation.
The intervention incorporates community-based, ageing-focused peer support groups to enable self-management, promote healthy behaviours, physical activity and combat loneliness for older adults.
Implementation is in part dependent upon existing public healthcare provision; effectiveness may be constrained by widespread health system resource limitations, as well as the financial constraints of the participant, affecting access to referrals and further specialized care.
The intervention focuses on the seven intrinsic capacity domains thought to have the greatest impact on functional ability, meaning other prevalent health conditions not directly related to these domains may be overlooked by the intervention.
Life expectancy is rising more rapidly in Africa than on any other continent.1 Whilst welcome, longevity alone is arguably not enough – the maintenance of functional ability, i.e., Healthy Ageing, is crucial.2 Healthy ageing, defined by the World Health Organization (WHO), is “the process of developing and maintaining the functional ability that enables wellbeing in older age”. Functional ability is the “health-related attributes that enable people to be and to do what they have reason to value”.3 This functional ability consists of a person’s intrinsic capacity within their environment, that is the composite of all the physical and mental capacities that an individual can draw on to function within their environment.2 Older people living in low- and middle-income countries (LMICs) are currently spending longer living with disability and dependence than those in high-income settings, leading to individual, family, and societal burdens.4 Furthermore, older people commonly experience multiple diseases, particularly when socioeconomically disadvantaged.5,6 The United Nations (UN) declaration of the Decade of Healthy Ageing 2021-2030 stated that now is the time to act to ensure the health of ageing adults, their families and communities.7
Sub-Saharan Africa (SSA) already has twice as many older adults as northern Europe, with projections increasing from 46 million in 2015 to 157 million by 2050.1 At age 60, in Africa, additional life expectancy is now 16 years for women and 14 for men, making older age a reality.1 According to the 2022 census, 4.6% (692,482) of Zimbabwe’s population were older persons, approximately 79% of whom were living in rural areas.8 In 2019, the WHO proposed a community-level model of integrated care for older people (ICOPE), a person-centred approach towards multi-dimensional assessment and management.3 ICOPE version 1.0 provided a framework for screening and assessment of six intrinsic capacities: locomotion, vision, hearing, cognition, psychological (mental health) and vital (nutritional) capacities.3 Recently, the second edition of ICOPE has added urinary incontinence as a seventh intrinsic capacity domain, together with greater emphasis on social care and support.9 As ICOPE has been developed for worldwide use, using an evidence-base largely derived from high-income settings, adaptation and contextualisation is needed before use, for the approach to be practical within a given healthcare economy.
In 2017, the Zimbabwean Ministry of Health and Child Care (MOHCC), in partnership with WHO and Age International, published the National Healthy Ageing Strategic Plan, describing a growing ‘epidemic of non-communicable diseases’, and highlighting a critical need for a healthy ageing strategy for Zimbabwe.10 The 2012 National Census Report showed that a quarter of disabled people in Zimbabwe were 60 years or older.11 Access to social and community support was low, largely due to the severe socio-economic challenges facing the country; low functional ability, partly due to musculoskeletal disorders, poor vision, and the inability to travel unaccompanied, further challenged access to care.
Historically, health systems in the region have been designed to provide episodic, reactive, curative healthcare (e.g., treatment of infection with antibiotics), with higher-level care provided by organ system-specific specialists. In contrast, older people need integrated, proactive care that integrates prevention and treatment for multiple conditions, or multimorbidity.12 Millions of older people are denied universal health coverage (UHC), i.e., the principle that everyone receives the full suite of necessary, quality health services without financial burden—because service provision relies solely on specialists.
Health services need to develop to meet the increasing demands of ageing populations. There is an opportunity to plan innovative, integrated models of non-specialist delivered care from the outset, rather than defaulting to historic, siloed approaches. Such interventions must be informed by context-specific research. The concept of healthy ageing is under researched in African populations.13 The Zimbabwean MOHCC have described two overarching goals in their vision of ‘an environment where healthy ageing is guaranteed to achieve functional ability of older persons’. These are to (i) create an enabling age friendly environment for the provision of quality and integrated health services for healthy ageing, and (ii) strengthen the provision of quality and integrated health services for healthy ageing.10
There is increasing evidence that community-based peer-to-peer support can improve uptake of healthcare for younger people in LMICs (e.g., Malawi,14 Mexico,15 Zambia16).17 In high-income settings, peer-to-peer support groups help maintain functional ability in older people in their own homes as they promote mobility and social engagement, support behaviour change, uphold autonomy, encourage physical activity and enhance community social support for older people.18–20 Little is known about community programmes specifically for older adults in low-resource settings. A peer-to-peer support model described by Geffen et al. (2019), in Cape Town, South Africa, was among the first of such programs to be developed and tested in an African country, targeting highly vulnerable, low-income older adults.21 Trained peer volunteers provided regular visits and phone calls, administered wellness screenings, made referrals, built friendships, encouraged social engagement and healthy living, and provided emotional and informational support.21 This model was acceptable and feasible in improving the wellbeing of older people. Similarly, peer-to-peer support models have been shown to be acceptable and feasible for older people with common mental health disorders in Zimbabwe.22 Peer-to-peer support models for older people in LMICs may offer a novel opportunity to complement healthcare to enable self-ownership of health management and promote healthy ageing. To date, no studies have integrated a peer-support model into a comprehensive healthy ageing intervention in an LMIC. This study will be the first to do so, hypothesising that such an approach can improve older adults’ functional ability by improving intrinsic capacity and the lived environment.
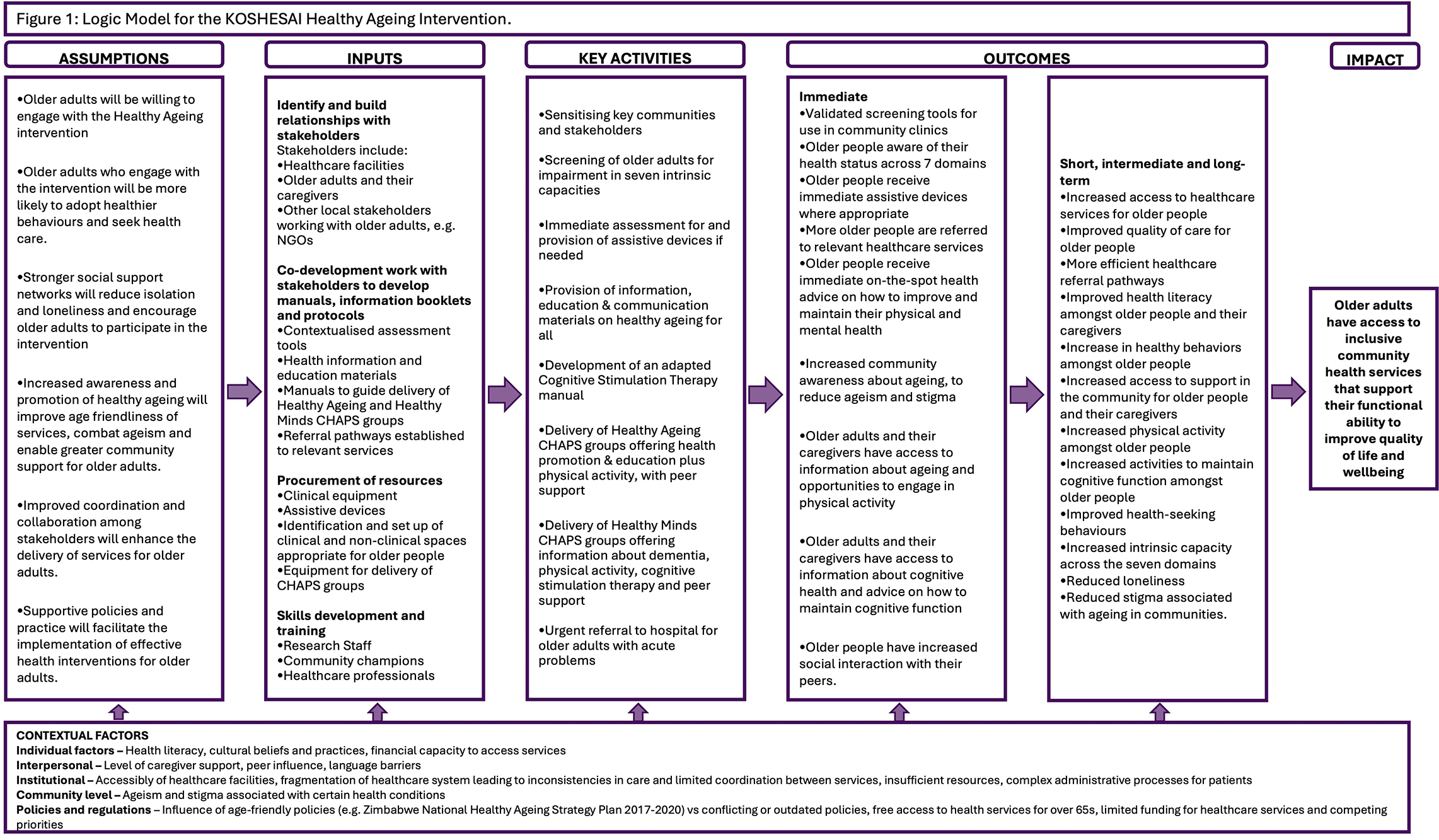
The Keeping Older people healthy, deSigning and evaluating effective HEalth Services to maintain functional AbIlity; KOSHESAI study provides a novel ‘healthy ageing’ clinic assessment, for older adults. Older adults in Zimbabwe are defined by the Old Persons’ Act as “a citizen of Zimbabwe aged sixty-five years or above, who is ordinarily resident”.10 Older adults will be screened for impairments in the seven intrinsic capacity domains, as set out by WHO ICOPE.3 If indicated, the team will provide immediate on-the-spot care, advice and/or referral.3 They will provide health promotion information and materials to support the adoption of healthy ageing behaviours and lifestyles. CHAPS groups will be developed, to which participants can be referred if eligible. The Healthy Ageing intervention is designed to be embedded within the current public healthcare system, being locally accessible, affordable, as well as clinically effective, so that should it prove effective, wider roll-out is feasible. Figure 1 presents a logic framework to underpin the design of the intervention. Table 1 applies the Template for Intervention Description and Replication (TIDieR) checklist to describe details of the intervention.23 Of note this healthy ageing assessment represents a significant departure from the prevalent disease-specific screening and treatment paradigms common in many LMIC primary care settings, such as for HIV, diabetes, and hypertension. While these conditions are important, established albeit siloed healthcare pathways already exist for these, thus the current intervention takes a holistic approach to assess intrinsic capacities specifically, aligning with the WHO ICOPE framework.
| No. | Item |
|---|---|
| BRIEF NAME | |
| 1. | KOSHESAI Healthy Ageing Intervention |
| WHY | |
| 2 | The KOSHESAI study intervention is centred on the concept of "Healthy Ageing", which promotes the maintenance of intrinsic capacity and hence functional ability with age. Its core rationale is to: The goal is to improve the health and wellbeing of older Zimbabweans by addressing intrinsic capacity deficits and providing a scalable model for healthy ageing interventions in similar settings. |
| WHAT | |
| 3 | The KOSHESAI intervention includes various information materials:
|
| 4. | Key KOSHESAI intervention procedures include:
|
| WHO PROVIDED | |
| 5 | The KOSHESAI intervention is delivered by a multi-disciplinary team, primarily featuring nurses, research assistants, CHAPS coordinators, CHAPS champions (lay volunteers), and a process evaluation team. All research staff will receive formal training. CHAPS champions are specifically trained using manuals provided to lead the groups. |
| HOW | |
| 6 | The KOSHESAI intervention is delivered face-to-face, involving individual assessments and personalized advice at clinics (or during home visits for those unable to attend) alongside group-based CHAPS sessions. |
| WHERE | |
| 7 | The KOSHESAI intervention will primarily occur in local polyclinics within urban Harare and rural Murehwa, Zimbabwe. Clinics will be renovated to create an age-friendly environment. Beyond the clinic, the intervention will extend into communities for CHAPS groups and home visits. |
| WHEN and HOW MUCH | |
| 8. | The intervention is designed to be delivered over a 4-month period. During this period, participants will have two clinic visits: a baseline assessment and a 4-month follow-up. Those referred to CHAPS groups will be offered 16 weekly (2 hours) sessions. |
| TAILORING | |
| 9. |
|
| MODIFICATIONS | |
| 10. ǂ | Any modifications will be reported when the results of the study are published. |
| HOW WELL | |
| 11. |
|
| 12. ǂ | Intervention fidelity will be reported when the study results are published. |
Patients and members of the public were involved in the development of the KOSHESAI study from the earliest stages of project conceptualisation. Their input has been instrumental in ensuring the study is culturally appropriate, feasible, and addresses the actual priorities of older people in Zimbabwe. Older people and caregivers were consulted prior to securing funding for this study, and subsequently in the design of study conduct, the assessments and proposed interventions.
In consultation with older adults, their caregivers, community gatekeepers in the study sites, and stakeholders (health professions, community-based organizations) working with older adults, we adapted the WHO ICOPE screening tools to ensure their relevance to our context, ensuring that the language is culturally sensitive. Consultative workshops also influenced the structure and content of the peer-to-peer support groups. The choice of primary and secondary outcomes was refined following consultation with the health professions of what would be clinically relevant, and feasible based on their daily practices.
To ensure inclusive recruitment and participation in the study, we asked older adults and stakeholders who had participated in workshops to spread the word of the study. Going forward, to enhance community engagement, eligible workshop participants—older adults and caregivers—will work alongside CHAPS facilitators to lead recruitment efforts within their own communities. The public also recommended that peer-to-peer support groups take place during times that do not conflict with local agricultural cycles or community events.
A key output of the study—the community engagement handbooks—will be distributed during community sensitisation days. These events will serve as a platform to promote health awareness. To ensure accessibility for all community members, we will provide health information in the form of short, visual fliers and pamphlets, translated into local languages. This approach ensures that dissemination is not just a one-way report, but a continuing conversation with the communities involved.
To develop, implement and evaluate an evidence-based, potentially sustainable, clinical framework for community-based non-specialist assessment and management of chronic impairments of ageing which impact intrinsic capacity and through this functional ability, to improve health and wellbeing of older people living in Zimbabwe.
• Develop and pilot test a healthy ageing clinic assessment for older adults that screens for deficits in the seven intrinsic capacities that impact functional ability, and provides contextually appropriate, locally accessible, affordable and effective interventions.
• Validate screening tests proposed by WHO ICOPE, to detect impairments in the seven intrinsic capacities, for use in the Zimbabwean population of older adults.
• Through a prospective hybrid type 2 implementation-effectiveness study in urban and rural settings, the study will: (i) estimate the short-term impacts on older adult health and wellbeing, as well as on individual intrinsic capacity impairments, (ii) understand through process evaluation the feasibility, fidelity of implementation, acceptability, quality and uptake of community healthy ageing peer-to-peer support group-based interventions and the influence of context, and (iii) evaluate the costs of implementing the assessment and interventions.
• Determine the prevalence of intrinsic capacity impairments detected by the healthy ageing clinic assessments.
• Gather all data and evidence needed to inform the development of a ‘Healthy Ageing Intervention Toolkit’, i.e., a guide for scale-up and maintenance of a structured, comprehensive, person-centred approach for non-specialist assessment and management of functional ability in older people in Zimbabwe. Refining the approach and its Theory of Change to finalise the optimal methods for the measurement of the impact of the programme when rolled out.
The study protocol is described following all recommendations established by 2025 Standard Protocol Items: Recommendations for Interventional Trials (SPIRIT).24
Community members and stakeholders were involved in the design of this research protocol. Using the 2019 WHO ICOPE framework as a starting point,9 the intervention was designed and contextualised following formative research conducted between December 2023 and December 2024 with a range of older people and their caregivers from the planned study settings, as well as key stakeholders, ageing-orientated non-governmental organisations (NGOs), and community-based organisations (CBOs). All community gatekeepers and leaders in the study communities were mapped and a network was established of KOSHESAI “champions”, constituting older people with and without recent health care experience(s), and key community leaders focused on older adult wellbeing. This formative work demonstrated that the planned healthy ageing assessments are highly desired by older people, likely to be feasible to implement, acceptable to stakeholders, and complementary to existing services. In urban Zimbabwe, it is expected that there is a substantial burden of unmet needs from previously untreated yet treatable intrinsic capacity impairments.25
The stakeholder engagement contributed not only to the adaptation of clinic assessments but also shaped the design of the components of the community intervention, and the development of information materials. Stakeholders provided valuable advice and emphasized the need for culturally appropriate nutritional guidance, advocating for the incorporation of locally sourced foods and traditional dietary practices to improve dietary behaviours. Stakeholders highlighted the importance of promoting physical activities that are both accessible and acceptable to older adults within the Zimbabwean context, with suggestions aimed at mitigating potential barriers to accessing services, e.g., clinic and community hall renovations to enable access for those living with disability. For mental health support, stakeholders stressed the need for integrated approaches that combine the Friendship Bench community-based support model22 with strengthened referral pathways to the Mental Health Gap (MhGAP) services26 embedded in the public health facilities. Key recommendations were to ensure the availability of appropriate and affordable assistive devices, such as walking sticks and reading glasses, to enhance mobility and sensory function.
Participatory workshops with older people and their caregivers found that older people were keen to learn more about their mental and physical health and about how they could improve their health over time. A CHAPS group intervention was co-designed with the older adults and stakeholders. CHAPS are designed to promote and maintain functional ability by facilitating self-management among older people. Older people, especially older men, were particularly interested in bladder health. Findings from workshops were used to co-create CHAPS facilitator handbooks, and the easy-to-understand information booklets on “healthy ageing” and bladder health (male and female specific versions). All booklets and handbooks were written in English and then translated into Shona, (additional Ndebele translation will follow). Booklets and handbooks were refined through focus group discussions (FGDs) with purposively selected men and women to ensure all relevant topics were covered and all information and images were understandable, appropriate, and acceptable.
To widely disseminate co-developed health information and promote healthy ageing, community education events were planned to be conducted in local community halls, during and after the recruitment period. These events will be open to the public and cover key topics relevant to older adult health, such as dementia and mental health, continence and sexual health, nutrition and physical activity, and abuse and neglect. Furthermore, outreach events will be organized at the one old age residential home in the study communities to maximise the reach of the intervention and evaluate it within an institutionalised care setting.
We hypothesize that a routine healthy ageing assessment and intervention addressing the seven core intrinsic capacity domains will have an immediate positive impact on the health and wellbeing of older people in Zimbabwe. This KOSHESAI intervention is underpinned by a logic model ( Figure 1) that outlines the causal pathways through which the intervention is expected to mediate its effect. This model delineates the intervention’s activities, outputs, and intermediate outcomes, while also considering contextual factors that may influence its implementation and effectiveness. The logic model was developed collaboratively, drawing on the expertise of the research staff, and individuals with in-depth knowledge of the Zimbabwean context. During participant recruitment, a ‘Theory of Change’ will be developed to make explicit the granular causal pathways leading to the outcomes of the healthy ageing intervention.
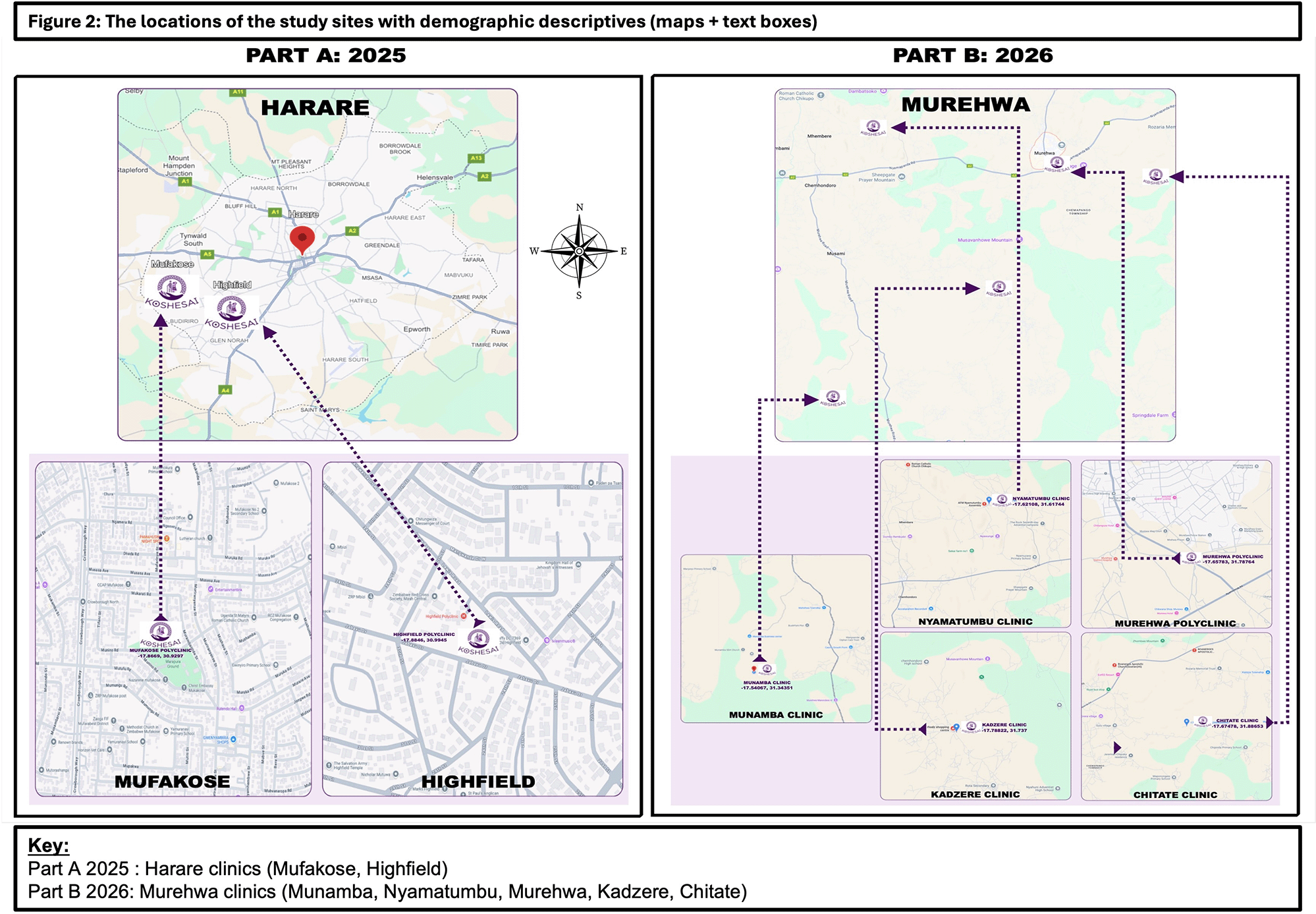
A prospective hybrid type 2 implementation-effectiveness study will recruit older adults age ≥65 years and follow them up for four months. The intervention will be delivered in local primary healthcare clinics (community-based public healthcare facilities providing a range of routine outpatient medical services) within urban and rural settings. This setting facilitates the integration of the intervention within the established primary care system, offering a local location for intervention delivery, aiming to enhance accessibility and convenience for participants. Older adults residing within two urban settings in Harare (Mufakose and Highfield) will be recruited in 2025. In 2026 recruitment will expand to four rural settings in Murehwa district (potential clinics include Nyamatumbu, Kadzere, Chitate, Munamba, and Murehwa) (see Figure 2 for locations of study sites). Study findings and the process evaluation from the urban setting, together with further community and stakeholder engagement and involvement in the rural setting, will inform intervention refinement ready for rural intervention in 2026.
Inclusion and Exclusion criteria
Adults aged ≥65 years based on photo identification, residing in the study areas will be included. Those with plans to relocate outside of the study area in the forthcoming four months, or with circumstances that would prevent them from returning for a 4-month follow-up appointment, will be excluded from the study.
Community sensitization
To enable participant recruitment a programme of community sensitization will be conducted in study communities using diverse approaches. A community team (research nurse and research assistants) will distribute study flyers, visit homes of potentially eligible individuals identified from the local offices of social welfare. Primary healthcare clinic staff will be able to refer older patients to the study team. Further methods will include community word-of-mouth, door-to-door house visits, and direct engagement at older adults’ social gathering points such as churches, beerhalls and betting halls. Participant identification will further involve referrals from CHAPS facilitators, community-based organizations, and previous study participants consenting to future contact for future studies.
The study clinic
Clinics have been renovated to ensure they offer an age-friendly environment, with improvements including ramps, grab bars in toilets, clearer signage (to toilets and study clinic assessment rooms), brighter lighting, and non-slip floor-proofing. Sanitation has been significantly improved by ensuring running water in toilets and the provision of cleaning detergents.
Consenting older adults will be screened for impairments in the seven intrinsic capacity domains, to identify the need for domain-specific interventions ( Table 2). Where needed, immediate on-the-spot interventions will be provided (e.g., ear syringing, fitting of walking sticks and/or reading glasses). Bespoke patient-specific health advice will be provided by trained nurses, relevant to the deficits identified, tailored to the participant’s specific health profile and risk factors, to promote healthy behaviours, self-management and health autonomy. All participants will be provided with a colour copy of the co-produced Healthy Ageing Booklet, designed to provide accessible and culturally relevant information on healthy ageing practices, which can be read by the older person and/or their caregiver(s) ( Figure 3).
| Intrinsic capacity domain | Screening tool | Condition | Evaluation tool | Primary outcome: Appropriate on-the-spot care or appropriate referral actioned | Secondary clinical outcome | |
|---|---|---|---|---|---|---|
| On-the-spot care | Appropriate referral | |||||
| Cognition | Recall & orientation | Cognitive Impairment | RUDAS ≤2227 | Patient and Carer Advice Referral for physical activity & CST28 | Attended first of 16-week Healthy Minds CHAPS group | WHODAS 2.029 HRQoL (EQ 5D-5L) |
| Psychological | PHQ-2 GAD-2 | Depression and Anxiety | PHQ-9 GAD-7 | Referral to local Friendship bench30 (if moderate or severe symptoms, or red flags referral to MhGAP nurse) | Attended first session with Friendship bench | HRQoL (EQ 5D-5L) |
| Vitality | Weight loss Appetite loss | Malnutrition | MNA (includes BMI) <8 out of 14 | Dietary counselling and advice +/- CHAPS referral re nutrition education | Attended first of 16-week Healthy Ageing CHAPS group | BMI +/- Reported food insecurity31 |
| BMI | Overweight | BMI | Dietary counselling and advice +/- CHAPS referral re nutrition education and physical activity | Attended first of 16-week Healthy Ageing CHAPS group | BMI | |
| Vision | Single question re. eye problems | Vision impairment | Tumbling E chart (near and distance vision with pin-hole correction) | Provided free reading glasses. Referral to refractionist Referral to eye hospital | Access to glasses. Cataract surgery performed or planned | Vision impairment Reported frequency of wearing glasses |
| Continence | 2 questions – urge & stress | Incontinence | ICIQ-IUSF, Bothersomeness of symptoms | Lifestyle and bladder training advice Pelvic floor muscle training (PFMT) | Adherence to bladder training and PFMT | ICIQ-IUSF
WHODAS 2.029 HRQoL (EQ 5D-5L) |
| Hearing | Whisper Test | Hearing impairment | hearWHO ≤40 (of 100) Otoscope | Wax removal (ear syringing) Hearing aid referral | Attended for hearing aid assessment | Hearing impairment & disability.32 Hearing aid use |
| Locomotion | Timed ‘get up and go’ test <20 seconds and Self-reported fall(s) | Falls, near falls, balance and/or gait impairment | Self-reported falls and near falls SPPB ≤533 | Provided advice on home adaptation Walking aid provision CHAPS referral re physical activity | Attended first of 16-week Healthy Ageing CHAPS group. | SPPB WHODAS 2.029 HRQoL (EQ 5D-5L) |
| Hip, knee and back pain | Brief pain inventory34 | Simple analgesia CHAPS referral re physical activity | Attended first of 16-week Healthy Ageing CHAPS group. | Reported pain WHODAS 2.029 HRQoL (EQ 5D-5L) | ||

Community healthy ageing peer-to-peer support groups (CHAPS)
Depending upon the deficits identified in the clinic, participants may be offered the opportunity to join a CHAPS group, either ‘Healthy Minds’ CHAPS if cognitive impairment is identified, or ‘Healthy Ageing’ if not. The CHAPS aim to promote and maintain functional ability by facilitating health promotion and self-management for older people. The two different types of CHAPS groups will be run to meet older people’s varying health needs: Healthy Minds CHAPS with focus on cognition and dementia, Healthy Ageing CHAPS with focus on improving mobility, nutrition, bladder health, and mental health. Healthy Ageing CHAPS, with 10-12 people in each group, will be split by gender as these groups will engage in sensitive discussions and exercises when addressing bladder health. Healthy Minds CHAPS groups, with five to eight people, will include both men and women. Each will be led by two community ‘champions’ (an older adult volunteer [age approximately ≥60 years], plus a younger adult volunteer [age 30-60 years]) who will be trained and supported by the multi-disciplinary project team. Where possible, champion pairings of an older and younger person are planned to harness diverse skill sets, relatability and organisational skills. Healthy Minds CHAPS champion pairings will have one man and one woman to represent the two genders in the groups. ‘How-to’ guides and manuals will guide the implementation of the CHAPS groups.
Referral to specialized services
Where indicated, research nurses will refer participants for further care, particularly for hearing impairment, visual impairment, depression and anxiety, and cognitive impairment ( Table 2). Referrals aim to link participants to specialized services for diagnosis, treatment, and ongoing management of identified health conditions. Transport costs incurred accessing referral services will be provided ($5 per older adult, +/- an additional $5 for a caregiver), addressing financial barriers to participation and promoting adherence to the intervention protocol. If a participant is found to be acutely unwell, they will be transferred to the local hospital emergency department.
Home visits
Adults unable to attend the primary healthcare clinic due to severe mobility impairments, or severe dementia will be seen at home. Home visits ensure all eligible participants can be assessed and receive the intervention, promoting inclusivity and addressing potential barriers to access. Assessments and interventions delivered during home visits will be adapted according to the individual health conditions and needs of the older adult.
The KOSHESAI study constitutes a multi-disciplinary team to ensure effective implementation and evaluation of the intervention. Two clinic teams, each led by a research nurse and composed of two research assistants, will manage participant recruitment, assessments, and clinic flow and logistics. A community team, also led by a research nurse, will lead community engagement and conduct home-based assessments. A CHAPS coordination team will oversee the training, monitoring, and evaluation of CHAPS champions during intervention delivery. A process evaluation team will evaluate implementation, impact mechanisms, and contextual influences. Another researcher will collect cost data in real-time. This structure integrates clinical service, community support, and rigorous evaluation. All staff will undergo a month-long training program, including classroom learning, scenario role-plays, and clinic ‘dry-runs’, covering ethical practices, study procedures, community engagement, data collection, intervention delivery, and data management.
Following training, a 15-day pilot phase will optimise assessment procedures and intervention delivery. Daily participant recruitment will gradually increase, allowing identification and mitigation of any logistical challenges and workflow inefficiencies in real-time. The process evaluation team will focus on key implementation parameters within the Medical Research Council (MRC) Process Evaluation framework.35 They will provide iterative, constructive feedback to the study team regarding the degree to which the intervention is delivered as specified in the protocol and identified barriers and facilitators to optimal clinic operations. Clinic observations, including participant waiting times, age-friendly communication, participants’ attitudes and response to the intervention, and overall operational efficiency, will be undertaken. In addition, the process evaluation team will collect time-and-motion data to quantify staff time allocation across the various clinic components. Dynamic feedback will enable iterative refinement of intervention delivery. Data collected in this phase will be included in the main study dataset.
All eligible participants will receive a clear verbal explanation and a Participant Information Sheet (PIS) in English or Shona, with time for questions before providing informed written or witnessed thumb-print consent, in line with the Declaration of Helsinki.36 Consent will cover assessments, interventions, clinical photography, audio recordings, data archiving, and future research contact. Older people lacking decisional capacity due to cognitive impairment will be eligible to participate, with surrogate consent obtained from their caregiver (consultee/proxy). If capacity is regained, standard consent will be sought directly from the participant.
Clinic
Data collection at baseline and 4-month follow-up visits will include researcher-administered questionnaires, and a series of physical assessments conducted in designated clinic rooms providing visual and auditory privacy. At baseline, the clinic flow will enable different researchers to conduct independent screening and validation assessments. All data will be captured directly into pre-programmed ‘off-line’ ODK forms, with data validation checks, on Samsung Galaxy tablets, which will be backed up at the end of each day.
At baseline data will be collected concerning sociodemographic factors (e.g., educational attainment, household income, marital status, food insecurity, caring responsibility), medical history (e.g. comorbidities, falls, disability,29,37 pain), medications, smoking and alcohol consumption, security and social support,38 activities of daily living (ADLs) and instrumental ADLs (iADLs),39 health-related quality of life (HRQoL) (using EQ 5D-5L which measures HRQoL over the previous two weeks40), and health expenditure in the previous 4-months. Where available, hand-held medical records will be interrogated to augment responses and determine historic events. Screening and validation assessments will be performed for all seven intrinsic capacity domains (cognition, mental health, nutrition, vision, hearing, continence, and locomotion) ( Table 2). No blood tests will be performed.
At the end of the clinic appointment the nurse will review the assessment. Where a deficit has been identified in one or more intrinsic capacities, they will offer on-the-spot advice and/or intervention and discuss goals and appropriate referral(s) according to the preferences of the older person. Potential interventions were listed in Table 2. The nurse will complete a semi-automated care plan, populated by the results of the assessments.
At 4-month follow-up data will be collected to determine new medical diagnoses, medication changes, changes in health behaviours, pain, disability, security and social support,38 ADLs and iADLs,39 and HRQoL.40 Data on out-of-pocket health-associated expenditure incurred by participants accessing the intervention, including any transport costs and opportunity costs, will be collected, as will data on referral uptake and experiences. The questionnaire will be refined during the intervention piloting phase and finalised before the 4-month follow-up. To minimise loss to follow-up, participants will receive a clinic reminder card with the follow-up date, and a reminder telephone call the day before their appointment date. In the case of missed appointments, visits will be rescheduled.
Process evaluation
We will conduct a mixed-methods process evaluation based on guidance from the MRC Process Evaluation framework.41 This evaluation aims to comprehensively assess the intervention’s implementation, mechanisms of impact, and the influence of contextual factors. The process evaluation will investigate intervention delivery, including acceptability, adoption, appropriateness, feasibility, fidelity, and intervention impact. Additionally, it will draw on implementation and behavioural science frameworks, including the Consolidated Framework for Implementation Research (CFIR),42 the Framework for Understanding Successful Interventions (FUSI), and the Capability, Opportunity, Motivation - Behaviour Change Model (COM-B).43 These frameworks will provide a theoretical basis for understanding intervention implementation from service providers’ perspectives (CFIR) and the intervention’s acceptability, uptake, and behavioural changes from the end-users’ perspectives (FUSI and COM-B).
The process evaluation will investigate several key domains: programme implementation, mechanisms of impact and context ( Table 3). Data will be collected at multiple time points, using multiple methods and sources, and in various locations (e.g., homes, community places, clinics) to ensure triangulation. Data collection tools will be developed in response to findings from formative work and guided by the theoretical frameworks. The process evaluation will remain flexible and dynamic throughout the study to adapt to emerging findings.
Quantitative data will provide insight into the reach and impact of implementation of the KOSHESAI intervention. At all intervention sites, routine metrics on program activity will be collected throughout the study period. This will include observations of variability of daily activities, such as reach, and time and motion measurements. Data on the reported uptake and acceptability of health services and CHAPS groups will be obtained after the initial screening and intervention visit and at the 4-month participant follow-up visit. CHAPS programme data will be collected, including data on CHAPS group set-up, meeting timelines and locations, participant attendance, and method and duration of travel to the meetings. The process evaluation will encompass the collection of data pertaining to linkage to care. This will involve monitoring communication and referral processes. The process evaluation team will also track intervention changes through intervention adaptation tracking forms.
Qualitative data collection for the KOSHESAI process evaluation will employ a range of methods to capture diverse perspectives and in-depth insights. Purposive and theoretically informed sampling will guide qualitative data collection, with consideration of service provider and participant characteristics (e.g., age, sex, engagement with the intervention). These methods will include observations of implementation activities, such as staff skills training, clinic screening and assessments, and CHAPS implementation, to provide contextual understanding of intervention delivery. In-depth interviews (IDIs) will be conducted with CHAPS facilitators, KOSHESAI implementation team members, service providers at referral points, and community stakeholders to explore their experiences and perceptions of service delivery. Focus group discussions (FGDs) and participatory workshops will be conducted with older adults and caregivers to understand their experiences and views of clinic screening and assessments, and their experiences of attending CHAPS groups. In-depth case studies will also be carried out with older adults and their family members to provide an in-depth understanding of pathways through care, including barriers and facilitators to access, acceptability, and behaviour change. These diverse qualitative methods will allow for a comprehensive exploration of the determinants of implementation, the intervention’s implementation outcomes, and mechanisms of impacts.
Economic evaluation
An economic evaluation will quantify resource use in developing, adapting, and delivering interventions across different care domains and determine participant out-of-pocket costs. Project expenditure data will be gathered during the start-up and implementation phases and used to estimate health system costs, including staff salaries, consumables, equipment, and transportation. In the absence of a Zimbabwean guide on discounting rates for costs and outcomes, all capital costs and any costs with a lifespan greater than the project life will be annualised using a 3-5% discount rate. Total costs will be allocated to different care domains using process evaluation data such as direct allocation based on information obtained from the finance department and time spent by staff on each domain, which will be collected using staff-time surveys. Research-specific costs will be identified and excluded from the analysis. Data on costs incurred by participants to access the healthcare services will be collected using a bespoke interviewer administered questionnaire. Participant costs will focus on both direct medical and non-medical costs. Medical costs will include healthcare services costs, such as hospital and clinic visits, medications, and diagnostic tests, while non-medical costs will encompass transportation, lost income for caregivers and food expenses during visits. This information will be combined to estimate unit costs per older person screened, condition identified, and person managed using both a health system and participant perspective. Key drivers of costs will be assessed; understanding will help inform the scale-up and financial sustainability of the Healthy Ageing assessment and intervention.
Baseline and follow-up measurements of HRQoL (using the digital, interviewer-administered, EQ 5D-5L40 - Shona or English versions) will be used to estimate quality-adjusted life years (QALYs), using the value set for Zimbabwe.44 The QALYs will be used as the economic evaluation outcome measure in the cost-effectiveness of the intervention as the cost per improvement in older persons’ HRQoL. Cost and cost-effectiveness estimates will be compared to similar programmes in the region and will inform programme replication, scalability, and financial sustainability for different implementing partners.
The primary outcome is the proportion of older adults identified as having a deficit in one or more of the seven domains of intrinsic capacity who receive appropriate on-the-spot care and/or complete appropriate referral to CHAPS and/or a health facility for treatment by follow-up at 4 months.
Secondary outcomes will include:
i) Diagnostic accuracy of screening tests for each of the seven domains of intrinsic capacity (baseline)
ii) Prevalence of intrinsic capacity impairments, co-morbidities and multi-morbidity (baseline)
iii) Yield of previously undiagnosed impairments/conditions (baseline)
iv) Change in clinical outcomes, including health-related quality of life and pain, and extent of intrinsic capacity impairments, overall, by domain of function and according to uptake of the intervention (4-months)
v) Process evaluation indicators including coverage, fidelity, acceptability, and intervention quality (4-months)
vi) Cost analysis of the intervention and its components (4-months)
i) Out-of-pocket expenditure attributable to taking up the intervention (4-months)
To have 3.5% precision to detect a 70% successful provision of appropriate on-the-spot care or complete appropriate referral to peer-to-peer community healthy ageing group support and/or a health facility for treatment, 659 older adults will need to be followed-up at 4-months. If 80% of older people screen positive in one of more intrinsic capacity domains and are therefore in need of an intervention, then 824 older people will need to be screened. This falls to 732 older people if 90% screen positive in one of more intrinsic capacity domains. Thus, each of the two urban primary healthcare clinics will recruit and screen to identify 363 older people with one or more intrinsic capacity impairments, to follow-up 330 participants at four months and allow for 10% loss to follow up.
A similar approach will be taken in the rural study, although refinement will be informed by the proportion screening positive for impairments, and who are lost to follow-up in the urban setting.
A mixed-methods approach will be utilized for data analysis, systematically processing collected data and drawing insights from both statistical and qualitative examinations. The subsections below detail the specific methodologies that will be applied to assess the intervention’s effectiveness and its operational aspects.
Statistical analysis
The primary analysis will be conducted separately, first for urban and second for rural settings. Secondary analyses will assess urban-rural differences. In the study settings a contemporaneous comparison group is not available as no routine screening is taking place, hence baseline assessments will provide the counterfactual for internal comparisons. Similarly, a before-after comparison is appropriate; since there is no treatment targeting healthy ageing in these settings, any reductions in prevalence of intrinsic capacity impairments between baseline and 4-month follow-up can be attributed to the healthy ageing intervention.
Counts and percentages, means and standard deviations (SD), medians and inter-quartile ranges (IQR) will be used to describe quantitative data. The ICOPE screening tools will be validated against assessment tools ( Table 2), calculating sensitivity, specificity, positive predictive value, and negative predictive value. Screening test results will be reported, as will the services delivered, and referrals made, overall and stratified by age, sex, and location. We will use descriptive analysis to describe clinic-level characteristics at each of the polyclinics.
The primary outcome is a single proportion which will be presented with a 95% confidence interval. Secondary outcomes which are measured at a single time point will be presented in a similar way. For outcomes which are measured at two or more time-points, a before-after analysis will be conducted comparing differences in measures between the two time-points. The unit of analysis will be the individual. For clinical outcomes which are measured at two or more time-points, the initial baseline visit will give the prevalence of undiagnosed and untreated intrinsic capacity impairments and chronic conditions which will represent the counterfactual. The proportion of undiagnosed and untreated intrinsic capacity impairments and chronic conditions at the 4-month follow-up visit will be formally compared to this counterfactual to estimate the effectiveness of the intervention in improving these clinical outcomes. We will assess health service and older-person-specific determinants of correct management of conditions at 4-months using multivariable linear and logistic regression.
Quantitative data collected as part of the process evaluation (e.g., program data, monitoring forms) will be analysed using descriptive statistics to assess intervention delivery, reach, and fidelity. The cost-effectiveness of community-based health checks will be evaluated from a health system and patient perspective by comparing both costs and health outcomes (measured in quality-adjusted life years, QALYs) against a counterfactual scenario of no health checks. The cost-effectiveness of various screening, assessment and treatment/referral scenarios will be modelled considering the underlying epidemiology, sensitivity and specificity of screening tests, and effectiveness of condition-specific interventions.
Qualitative Analysis
Qualitative data will be analysed using an inductive thematic analysis.45 Given the study’s focus on applied health research and the need for a structured approach to analyze data across cases and sites, we will also incorporate elements of the Framework Method46 to aid in data management and comparison. Analysis will be informed by the CFIR and FUSI frameworks to understand service provider and user perspectives on implementation; and the COM-B model to identify factors influencing behaviour change in older adults.
Integration of findings
Qualitative and quantitative data will be triangulated using a convergent parallel study design.47 Findings will be integrated at the level of interpretation using a narrative approach.47 This will provide a richer, more nuanced understanding of how the intervention is being experienced and delivered. The findings will provide evidence to support development of the Healthy Ageing Intervention Toolkit and inform potential future sustainable and scalable implementation by health care providers should the intervention prove successful.
Ethical approval for this study was obtained from the ethics committee of the Medical Research Council of Zimbabwe (reference MRCZ/A/3077;15 December 2023).
Data protection and management
Data protection will be strictly observed. After the study completion, data will be stored at data.bris following General Data Protection Regulations (GDPR). Third party researchers wishing to access individual data records will be able to apply following processes outlined at http://www.bristol.ac.uk/staff/researchers/data/accessing-research-data/, subject to a data transfer agreement and informed consent procedures regarding use of anonymised data by other researchers. Data for sharing will be anonymised so that they contain no information that could directly identify any of the participants. Data users will need to acknowledge data sources and ensure regulatory requirements are met: The Medical Research Council of Zimbabwe (MRCZ), expects that a Zimbabwean co-author be included in all publications resulting from data collected on Zimbabwean human subjects.
The KOSHESAI study represents a substantial effort to contextualize, implement and evaluate a healthy ageing intervention within the challenged socio-economic and healthcare context of Zimbabwe. While the WHO ICOPE framework3 provides a valuable foundation, it is essential to tailor assessments and interventions developed in high-income countries to ensure their relevance and effectiveness in LMICs. The KOSHESAI study recognizes this necessity and through stakeholder engagement, it aims to co-produce and adapt the approach to the specific needs and resources of the Zimbabwean population and healthcare economy.
The study employs a rigorous hybrid type 2 implementation-effectiveness design,48 enabling the simultaneous evaluation of both the implementation process and the intervention’s impact. This approach will provide a comprehensive understanding of not only whether the intervention works, but also how and why it works (or does not) in a real-world setting. Beyond assessing the intervention’s effectiveness and implementation, this study will also contribute valuable data on the prevalence and burden of deficits across the seven WHO ICOPE domains, among older adults in Zimbabwe. This will fill a critical data gap in LMICs, informing public health planning for ageing populations.
The incorporation of CHAPS groups represents a novel ageing intervention in this setting, with the potential to enhance self-management, promote healthy ageing behaviours, and enhance wellbeing and sustainability. While community-based peer support models have shown promise in various health interventions globally, including for HIV and chronic disease management in LMIC,49–51 and for mental health,22,52,53 their integration within the ICOPE framework for healthy ageing in this specific setting is novel. Hitherto, the model in South Africa,21 which was among the first peer-to-peer support programs for older adults developed in an African country, has paved the way, and KOSHESAI extends this important work. Peer support is a low-cost, accessible, and potentially scalable model54 to support healthy lifestyles across the continent, whether integrated within an ICOPE-based health check or independently thereof.
A detailed process evaluation, guided by the MRC framework41 and implementation science frameworks (CFIR, COM-B and FUSI),42,43 will allow us to iteratively refine the intervention during its implementation and provide data on its practical deployment, fidelity, and contextual appropriateness among older adults, community members, and healthcare providers, informing future scale-up. Additionally, the integration of a cost evaluation will provide crucial data on the economic implications of implementing the healthy ageing intervention, which is particularly vital in a resource-constrained setting like Zimbabwe. This will inform future resource allocation and policy decisions, contributing to the sustainability and scalability of similar programs in LMICs.
The inclusion of both urban and rural settings in the study design will enhance the generalizability of findings, ensuring applicability across diverse contexts. This is crucial as healthcare access, infrastructure, and social determinants of health often vary significantly between these areas. As 62% of people in East and Southern Africa and 61.4% of people in Zimbabwe55 live in rural settings, the study design enables potential national and regional scale-up. The study will inform the development of a context-specific ‘Healthy Ageing Intervention Toolkit’, which will provide guidance for a structured, comprehensive, person-centred approach for non-specialist assessment and management of functional ability in older people in Zimbabwe. In settings like these, where there are no specialist nurses or physicians in aged care, providing standardized protocols and clear guidelines within a toolkit can significantly enhance the quality and consistency of integrated care delivered by nurse-led clinics. Upskilling staff in this area facilitates task-sharing to strengthen primary healthcare systems to proactively provide healthcare services to older adults.56 Developed tools serve as practical resources for training, capacity building, and governance activities, ensuring that evidence-based healthy ageing practices, like those promoted by the WHO’s ICOPE framework, are translated effectively into routine care.
It is important to acknowledge the potential limitations and challenges of this study. Implementing a multi-faceted intervention within resource-constrained healthcare settings presents inherent complexities. As shown when introducing integrated HIV care services,57 integrating screening for intrinsic capacity impairments among older adults into an already short-staffed and overstretched health system poses a significant challenge; it adds to existing workloads and will require specific training. Furthermore, a critical challenge stems from societal and professional perceptions of ageing, which often manifest as ageism. Ageing is commonly viewed as a normal part of life rather than a phase with distinct health needs. Moreover, older people are frequently viewed as having diminished economic value, a misguided notion given that a substantial proportion serve as primary caregivers for grandchildren,58,59 they contribute significantly to household economies and have been shown to constitute a substantial number of senior healthcare workers (nurses) in the country.60 This bias can lead to the functional decline in older adults not being prioritized as a pressing concern by healthcare workers amidst competing demands, potentially impacting the enthusiasm for and uptake of new screening protocols.
Beyond these systemic issues, ageism, disability, and stigma present significant challenges to the health and wellbeing of older adults and can create barriers to accessing healthcare and social services.61 The KOSHESAI study explicitly acknowledges these challenges and has curated strategies to mitigate their impact. These strategies include: (1) integrating specific messages into community sensitization activities to raise awareness and challenge negative stereotypes, (2) ensuring the intervention is designed and delivered in a manner that is accessible and inclusive of individuals with disabilities, and (3) promoting empowerment and autonomy among older adults to counter the effects of stigma.
Financial constraints faced by participants may well impact uptake of referrals, thereby limiting the impact of the intervention. This broad systemic challenge, alongside existing health system barriers, may constrain the real-world effectiveness of the health assessment if identified needs cannot be addressed due to socio-economic factors.60 Furthermore, the long-term sustainability of the CHAPS intervention beyond the study period remains contingent on fostering robust community ownership and successful integration into existing health structures. A limitation is that the broad, nurse-led assessment, while designed for wide reach and feasibility, may not detect all serious or subtle health conditions, particularly those outside the seven intrinsic capacity domains, and the study’s 4-month follow-up period may not capture the emergence or progression of all such conditions.
The KOSHESAI study is a pragmatic approach to developing and evaluating a novel context-specific healthy ageing intervention within the socio-economic and healthcare setting of Zimbabwe. The study represents the first implementation-effectiveness study of a WHO ICOPE3 based healthy ageing intervention in Africa. It will provide critical evidence to inform successful adaptation and operationalization of healthy ageing interventions, suitable for use in LMICs, which are potentially scalable non-specialist dependent models of community-based healthcare delivery. Findings will contribute substantially to this decade of ‘healthy ageing’,7 offering a transferable blueprint for enhancing the health and wellbeing of older adults facing similar systemic challenges worldwide.
All study procedures will adhere to the principles of ethical research involving human participants, including informed consent, confidentiality, and the right to withdraw. Particular attention will be paid to safeguarding older adults, ensuring their well-being throughout the study period. Data will be stored securely and managed according to data protection regulations. To ensure the dissemination of study findings, results will be published in peer-reviewed journals, presented at national and international conferences, and shared with relevant stakeholders, including healthcare providers, policymakers, and community organizations. Anonymized data will be deposited in a data repository to promote data sharing and facilitate future research.
No underlying data are associated with this article, as it presents a protocol for a study before starting data collection. The study instruments, including the adapted ICOPE screening tool, the Peer-to-Peer Support Group manual, and focus group discussion guides, will be made available at data.bris once they have been evaluated as part of the proposed program of work (and refined as needed).
Upon completion of the study, the investigators will make the de-identified datasets (including participant demographics, functional ability scores, and quality of life measures) available at https://data.bris.ac.uk/data/ to researchers with appropriate ethical and governance permissions in place, as necessitated by the Medical Research Council of Zimbabwe. In this way data will be shared under a CC-BY 4.0 license to allow for replication and reuse. Any qualitative data that could potentially identify participants will be handled in accordance with the ethical approvals obtained, and only fully anonymized transcripts will be shared.
The authors thank the participants (older adults, caregivers, and stakeholders) who took part in both the designing and implementation of the study, together with the Ministry of Health and Child Care (MoHCC) in Zimbabwe for their support.
Provide sufficient details of any financial or non-financial competing interests to enable users to assess whether your comments might lead a reasonable person to question your impartiality. Consider the following examples, but note that this is not an exhaustive list:
Sign up for content alerts and receive a weekly or monthly email with all newly published articles
Register with NIHR Open Research
Already registered? Sign in
If you are a previous or current NIHR award holder, sign up for information about developments, publishing and publications from NIHR Open Research.
We'll keep you updated on any major new updates to NIHR Open Research
The email address should be the one you originally registered with F1000.
You registered with F1000 via Google, so we cannot reset your password.
To sign in, please click here.
If you still need help with your Google account password, please click here.
You registered with F1000 via Facebook, so we cannot reset your password.
To sign in, please click here.
If you still need help with your Facebook account password, please click here.
If your email address is registered with us, we will email you instructions to reset your password.
If you think you should have received this email but it has not arrived, please check your spam filters and/or contact for further assistance.
Comments on this article Comments (0)